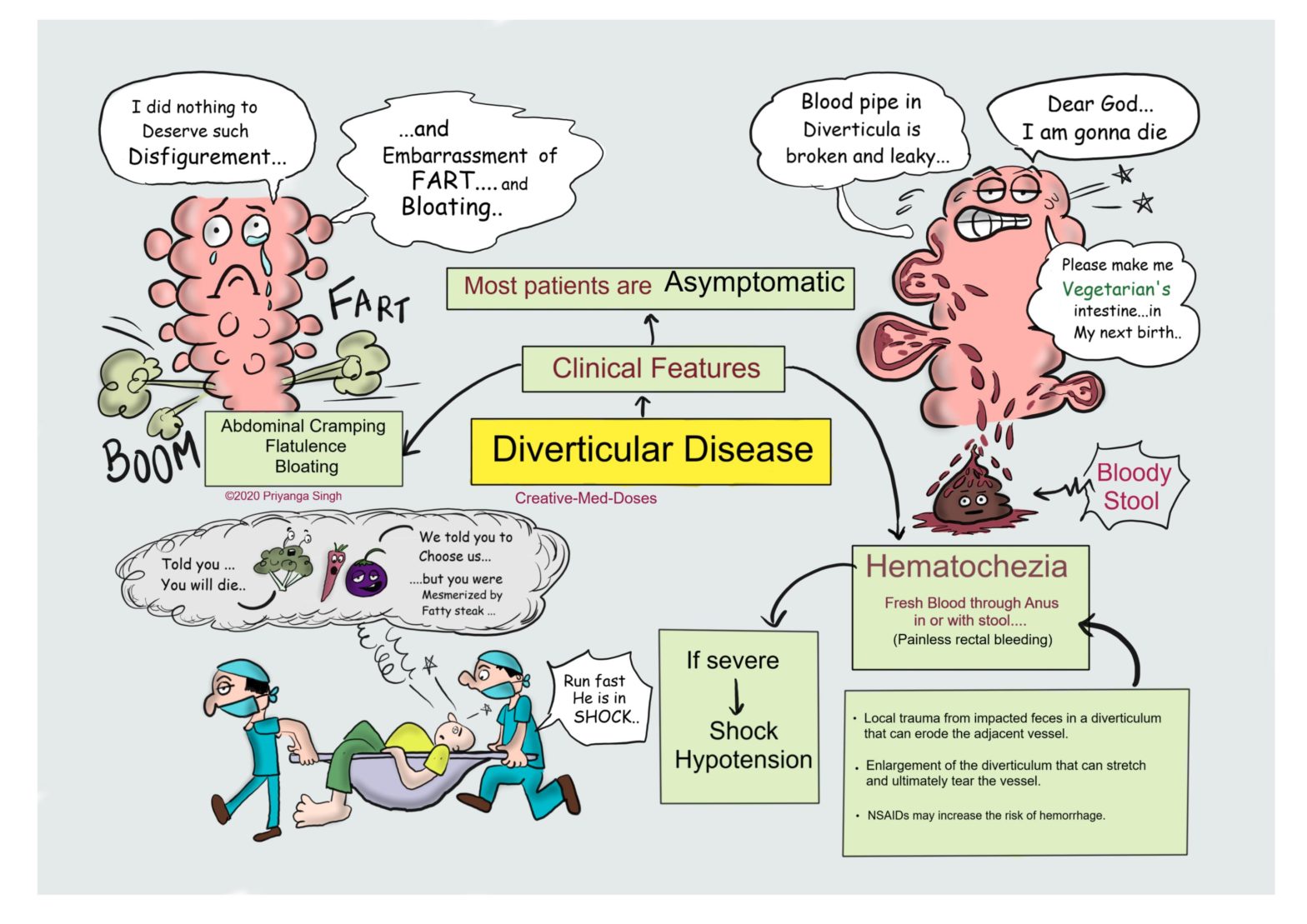
Diverticulitis is a condition that affects the digestive system, specifically the colon. It occurs when small, bulging pouches (diverticula) in the colon become inflamed or infected. While the exact causes of diverticulitis are not fully understood, diet, lifestyle, and certain medical conditions can play a significant role. One area of interest is the relationship between diverticulitis disease and alcohol. This blog post will delve into the intricacies of diverticulitis, its symptoms, causes, and the impact of alcohol consumption on this condition.
Understanding Diverticulitis
Diverticulitis is a common condition that primarily affects older adults. It is characterized by the formation of small, bulging pouches (diverticula) in the lining of the digestive system. These pouches can become inflamed or infected, leading to symptoms such as abdominal pain, fever, and changes in bowel habits. While diverticulitis can be managed with lifestyle changes and medication, severe cases may require hospitalization and surgery.
Symptoms of Diverticulitis
The symptoms of diverticulitis can vary from mild to severe. Common symptoms include:
- Persistent abdominal pain, often on the lower left side
- Fever and chills
- Nausea and vomiting
- Changes in bowel habits, such as constipation or diarrhea
- Abdominal tenderness
In severe cases, diverticulitis can lead to complications such as abscesses, fistulas, intestinal blockages, and perforation of the colon. If you experience any of these symptoms, it is important to seek medical attention promptly.
Causes of Diverticulitis
The exact causes of diverticulitis are not fully understood, but several factors are believed to contribute to its development. These include:
- Low-fiber diet: A diet low in fiber can lead to constipation and straining during bowel movements, which can increase pressure in the colon and contribute to the formation of diverticula.
- Aging: The risk of developing diverticulitis increases with age, as the colon walls can weaken over time.
- Obesity: Being overweight or obese can increase the risk of diverticulitis.
- Smoking: Smoking can weaken the colon walls and increase the risk of diverticulitis.
- Sedentary lifestyle: A lack of physical activity can contribute to constipation and increase the risk of diverticulitis.
Diverticulitis Disease and Alcohol
The relationship between diverticulitis disease and alcohol is a topic of ongoing research. While moderate alcohol consumption may not directly cause diverticulitis, excessive alcohol intake can exacerbate symptoms and complications. Alcohol can irritate the lining of the digestive system, leading to inflammation and increased risk of infection. Additionally, alcohol can interfere with the absorption of nutrients, which can further weaken the immune system and make it more difficult to manage diverticulitis.
Studies have shown that heavy alcohol consumption can increase the risk of developing diverticulitis and other gastrointestinal disorders. Alcohol can also interact with medications used to treat diverticulitis, potentially reducing their effectiveness. Therefore, it is important for individuals with diverticulitis to limit their alcohol intake and consult with their healthcare provider about any potential interactions with their medications.
Managing Diverticulitis
Managing diverticulitis involves a combination of lifestyle changes, medication, and in some cases, surgery. Here are some key strategies for managing diverticulitis:
Dietary Changes
A high-fiber diet is essential for managing diverticulitis. Fiber helps to soften stools and reduce pressure in the colon, which can help prevent the formation of diverticula and reduce the risk of inflammation. Foods rich in fiber include:
- Fruits and vegetables
- Whole grains
- Legumes
- Nuts and seeds
It is also important to stay hydrated by drinking plenty of water throughout the day. This can help to soften stools and prevent constipation.
Medication
Medications are often prescribed to manage the symptoms of diverticulitis and prevent complications. Common medications include:
- Antibiotics: To treat infections
- Pain relievers: To manage abdominal pain
- Stool softeners: To prevent constipation
In severe cases, hospitalization may be required for intravenous antibiotics and fluids.
Lifestyle Changes
In addition to dietary changes and medication, lifestyle modifications can help manage diverticulitis. These include:
- Regular exercise: To promote bowel regularity and reduce the risk of constipation
- Avoiding smoking: To reduce the risk of diverticulitis and other gastrointestinal disorders
- Limiting alcohol intake: To reduce inflammation and prevent complications
Surgery
In severe cases of diverticulitis, surgery may be necessary to remove the affected portion of the colon. This procedure, known as a colectomy, can help to prevent complications and improve quality of life. Surgery is typically reserved for cases where medication and lifestyle changes are not effective.
📝 Note: It is important to consult with a healthcare provider before making any significant changes to your diet or lifestyle, especially if you have a pre-existing medical condition.
Preventing Diverticulitis
While diverticulitis cannot always be prevented, there are several steps you can take to reduce your risk. These include:
- Eating a high-fiber diet
- Staying hydrated
- Exercising regularly
- Avoiding smoking
- Limiting alcohol intake
Regular check-ups with your healthcare provider can also help to detect and manage diverticulitis early, reducing the risk of complications.
Complications of Diverticulitis
If left untreated, diverticulitis can lead to several complications. These include:
- Abscesses: Collections of pus that can form in the colon
- Fistulas: Abnormal connections between the colon and other organs
- Intestinal blockages: Obstructions in the colon that can prevent the passage of stool
- Perforation of the colon: A hole in the colon that can lead to infection and sepsis
Prompt medical attention is essential to prevent these complications and manage diverticulitis effectively.
When to Seek Medical Attention
If you experience any of the following symptoms, it is important to seek medical attention promptly:
- Severe abdominal pain
- Fever and chills
- Nausea and vomiting
- Changes in bowel habits
- Blood in the stool
These symptoms can indicate a serious condition that requires immediate medical attention.
Living with Diverticulitis
Living with diverticulitis can be challenging, but with the right management strategies, it is possible to lead a healthy and active life. Here are some tips for living with diverticulitis:
- Follow a high-fiber diet
- Stay hydrated
- Exercise regularly
- Avoid smoking
- Limit alcohol intake
- Attend regular check-ups with your healthcare provider
By following these tips and working closely with your healthcare provider, you can manage diverticulitis effectively and improve your quality of life.
Diverticulitis is a common condition that can be managed with lifestyle changes, medication, and in some cases, surgery. The relationship between diverticulitis disease and alcohol highlights the importance of limiting alcohol intake to reduce inflammation and prevent complications. By following a high-fiber diet, staying hydrated, exercising regularly, avoiding smoking, and attending regular check-ups, you can manage diverticulitis effectively and improve your overall health.
Related Terms:
- does alcohol cause diverticulitis
- diverticulitis and beer
- diverticulitis foods to avoid alcohol
- diverticulitis and alcohol mayo clinic
- how does alcohol affect diverticulosis
- diverticulitis and alcohol use